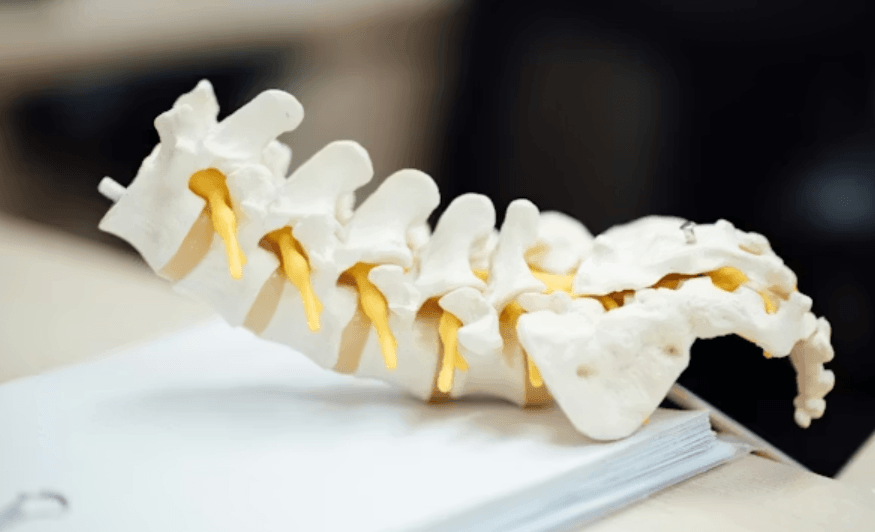
Chronic back and joint pain affects millions of people every year, quietly disrupting their daily life in ways that are easy to underestimate. Many live with persistent discomfort for months before seeking proper medical attention. By then, the underlying condition has often progressed to cause even more pain. Understanding what drives these conditions and how to treat them is the first step toward getting meaningful, lasting relief.
Musculoskeletal pain rarely has a single cause. It builds gradually through poor posture, sedentary habits, age-related degeneration, and sometimes underlying inflammatory conditions that go undetected for years. Seeking evaluation from an orthopedician specialist in Ranchi gives patients access to structured diagnosis rather than guesswork. The right clinical assessment identifies whether pain originates from the spine, joints, or damaged soft tissue.
When the Body Starts Sending Signals You Cannot Ignore
The Pattern Behind Persistent Pain: Chronic back and joint pain often begins with minor structural issues that go unaddressed for far too long. Over time, cartilage breakdown, disc compression, or muscle imbalances create persistent inflammatory responses that worsen gradually. What starts as occasional stiffness can become a condition that limits mobility, disrupts sleep, and affects mental well-being, making early clinical attention genuinely critical for long-term recovery.
The Problem With Home-Based Pain Management: Over-the-counter relief can mask symptoms temporarily, but does nothing to correct underlying damage. Many patients spend months relying on heat pads, generic tablets, and rest, only to find their condition worsening steadily. Without addressing the structural or inflammatory cause, the pain cycle continues and can lead to permanent joint deterioration, narrowing the window for conservative treatment options.
What a Proper Diagnosis Actually Changes
Reading Beyond Surface Symptoms: Accurate diagnosis of back and joint pain goes well beyond a physical examination. Imaging studies, including X-rays and MRI scans, provide detailed views of degenerative disc disease, joint space narrowing, and nerve compression. This layered approach helps clinicians build a treatment plan that targets the actual source of pain rather than surface-level expressions of it alone.
Conditions That Specialist Evaluation Regularly Uncovers: Many patients are surprised to learn the exact nature of their condition once proper imaging and clinical evaluation are complete. A wide range of musculoskeletal disorders share overlapping surface symptoms yet require distinct treatment approaches. Identifying each condition accurately is what determines whether a patient recovers fully or continues managing discomfort indefinitely without real progress.
- Lumbar disc herniation, where displaced disc material presses against nerve roots, causing radiating leg or hip pain.
- Osteoarthritis of the knee or hip, characterised by progressive cartilage loss and increasing stiffness following periods of rest.
- Ankylosing spondylitis, a chronic inflammatory spinal condition that can gradually lead to vertebral fusion over time.
- Sacroiliac joint dysfunction, which mimics lower back pain but originates from the joint connecting the spine to the pelvis.
- Cervical spondylosis, a degenerative neck condition causing referred pain that radiates into the shoulders and upper arms.
Why Early Staging Shapes the Treatment Outcome: The stage at which a condition is diagnosed directly shapes the treatment pathway available to the patient. Early-stage arthritis or disc compression responds well to physiotherapy, targeted exercises, and anti-inflammatory medication. Advanced degeneration may require minimally invasive intervention or surgical correction. Waiting too long often removes the least intensive treatment options from the table entirely.
The Role Daily Habits Play in Chronic Pain Progression
How Sedentary Behaviour Accelerates Joint Wear: Prolonged sitting, poor ergonomic habits, and repetitive physical strain contribute significantly to the progression of back and joint conditions over time. People who spend extended hours without adequate lumbar support, or who lift heavy loads without proper technique, place disproportionate stress on spinal structures and joint surfaces. These patterns are modifiable but require guided professional correction rather than self-directed adjustments.
Weight and Its Direct Impact on Joint Health: Excess body weight places measurable additional stress on weight-bearing joints such as the knees, hips, and lumbar spine. Research consistently shows that patients with elevated body mass experience faster cartilage degradation and more severe pain over time. Weight management is not a secondary consideration in orthopaedic care but an active component of any effective, lasting treatment plan.
See also: What Actually Changes in Your Water Pressure
How Orthopaedic Specialists Build a Path to Recovery
Treatment That Starts With Structured Assessment: Orthopaedic management is not a single approach but a layered process that adapts as the patient’s condition evolves. Clinicians typically begin with conservative care, including physiotherapy, bracing, corticosteroid injections, and structured exercise programmes. This phase addresses pain, improves joint stability, and builds a clearer picture of how the condition responds before any further clinical intervention is considered.
When Surgical Intervention Becomes Necessary: Some conditions do not respond adequately to conservative management, particularly those involving significant synovial inflammation, structural instability, or severe nerve compression that limits daily function. In these cases, surgical options such as arthroscopy, spinal decompression, or joint replacement are considered. Modern orthopaedic surgery has become considerably less invasive, with shorter recovery periods and better long-term functional outcomes than older procedural approaches.
Rehabilitation as the Third Phase of Recovery: Surgical or non-surgical treatment is rarely the end of an orthopaedic care pathway. Structured rehabilitation restores strength, corrects movement patterns, and rebuilds joint confidence over time. Patients who engage fully with post-treatment programmes consistently achieve better long-term outcomes than those who stop care once acute pain reduces. Recovery works best when it is patient-driven and clinically supervised throughout.
Pain Is Not Something to Simply Live With
Chronic back and joint pain is manageable when addressed through the right clinical framework rather than through improvised home care. Seeking orthopaedic evaluation early gives patients access to evidence-based treatment that targets root causes rather than surface discomfort. Whether the condition is arthritic, spinal, or structural, specialist-guided care offers a far more reliable path to regaining full physical function. Consult an orthopaedic specialist today to begin a structured assessment and recovery plan.